News
Clearlake City Manager Alan Flora had reported Pace’s plans to resign to the Clearlake City Council during its Thursday night meeting. Flora had been in a meeting earlier in the day in which Pace had announced his intentions to leave his post, as Lake County News has reported.
On Friday, the county of Lake released a statement from Pace, who has served as Lake County’s Public Health officer for the past 16 months.
He said the decision to resign was “a very difficult one” and his official last day in the role will likely be in mid-April, but he expects to provide support over a longer period if he’s needed.
Pace, who worked for more than 20 years in family medicine, said he’s returning to clinical practice in the coming months.
“Serving Lake County during the COVID-19 pandemic has been one of the most rewarding experiences and greatest challenges of my career. Particularly over these past 11 months, I have given all I had the capacity to give. I sought to listen to the needs of local residents, and provide safety measures and other health recommendations that best reflected the available science, knowing they would often be widely criticized,” Pace said.
Board of Supervisors Chair Bruno Sabatier said he found out early this week that Pace was planning to leave.
“Dr. Pace feels the pandemic has reached a new chapter where his skill sets aren't as necessary or needed as they were early on. Logistics and organization is what is needed currently to ensure appropriate and efficient deployment of the vaccine,” Sabatier told Lake County News.
Sabatier said that the board would discuss its next steps with regard to Pace’s resignation during its Tuesday meeting.
On Friday, Pace reported the same, noting that at that time the board will discuss its strategy to select his successor.
Under state law, California counties are required to have Public Health officers.
The news comes as Lake County this week reached 40 COVID-19 related deaths, with more than 3,000 confirmed cases, based on Lake County Public Health statistics.
Pace said his greatest sadness is leaving the relationships he’s developed in the Public Health officer role, he expressed his gratitude to the supervisors, and county administration, department heads and staff, and thanked the many people who have supported his work in Lake County.
“The team at the Health Services Department, under Denise Pomeroy’s capable leadership, is truly remarkable. I have seen people at all levels of the organization do incredible things, and that lends great hope for the future,” he said.
“While my primary responsibility has been to protect the health of Lake County’s communities, it has been truly heartbreaking to see the many types of consequences that have come for individuals and businesses in the past year,” he continued.
He said the nearly 48,000 deaths from COVD-19 in California alone, “have shook every one of us; no one can be unaffected.”
Pace also noted the other impacts of the pandemic, including children missing a full year of in-person instruction and the social barriers to educational attainment being greatly exacerbated, and the “still-mounting consequences to businesses of all sizes.”
“We also continue to count the costs associated with mental health effects of the rapid social changes of the past year, and the social isolation that has too often stemmed from “social distancing” mandates,” he said.
“Now, we stand at an inflection point in our pandemic response. The high boil of the initial crisis has transitioned toward a sustained, long-term-focused response that will require intensive partnership with the state and other organizations in our communities. Our COVID-19 vaccination effort, so key to a return to some kind of ‘normal,’ is still in the early phases, but there is hope supply and distribution will continue to ramp up in the coming months,” Pace said.
“I truly believe better days are ahead for Lake County,” Pace concluded.
Email Elizabeth Larson at
Dr. Gary Pace made the announcement in a Thursday morning meeting with local leaders, Clearlake City Manager Alan Flora told Lake County News.
Flora, who was present at the Thursday meeting where Pace stated his resignation plans, reported the situation to the Clearlake City Council on Thursday night.
Flora, who called the situation “a little disappointing,” said the county will be recruiting for a new Public Health officer over the next few months, and that Pace had indicated he would be around until some point in April.
Pace, who has been Lake County’s Public Health officer for 16 months, did not respond to a Thursday evening email from Lake County News regarding his plans to leave the county’s employ.
Separately, Board of Supervisors Chair Bruno Sabatier confirmed to Lake County News on Thursday night that Pace is resigning.
Sabatier said a discussion about how the board will move forward regarding the Public Health officer position will be on the supervisors’ Tuesday agenda.
California state law requires counties to have Public Health officers to enforce local health orders and ordinances, and state regulations and statutes.
Tuesday also is the day that Pace is scheduled to give the board another COVID-19 update and discuss the work of his recently convened COVID-19 Ethics Ad Hoc Committee, which is to address vaccine equity and prioritization.
The Board of Supervisors appointed Pace, a Sonoma County resident, Public Health officer on a permanent basis in October 2019, after he had filled the position for two months on an interim basis.
Previous to his interim service in 2019, he also had been Lake County’s interim Public Health officer from late 2017 to spring of 2018 and from the summer of 2018 until fall of 2018, as well as Mendocino County’s Public Health officer, as Lake County News has reported.
At the time of his permanent appointment, Supervisor Tina Scott, then chair of the board, lauded Pace as “a truly thoughtful individual and excellent medical mind” who she said “will help us progress toward a healthier Lake County.”
Five months later, Pace was in charge of Lake County’s COVID-19 response, taking a wide variety of actions including issuing a shelter in place order for county residents and a followup order that, for a time, closed Clear Lake and other local waterways to avoid drawing visitors, and also closed lodging facilities to anyone who wasn’t in health care worker or other essential fields.
In his report to the council on Thursday night, Flora said of Pace, “Overall he’s been a good partner with the city and we’ve enjoyed working with him, and he’s always been responsive to the concerns that we’ve had. So we wish him the best.”
In related news, on Wednesday the county of Mendocino announced the appointment of Mary Alice Willeford as that county’s interim Public Health director.
Email Elizabeth Larson at

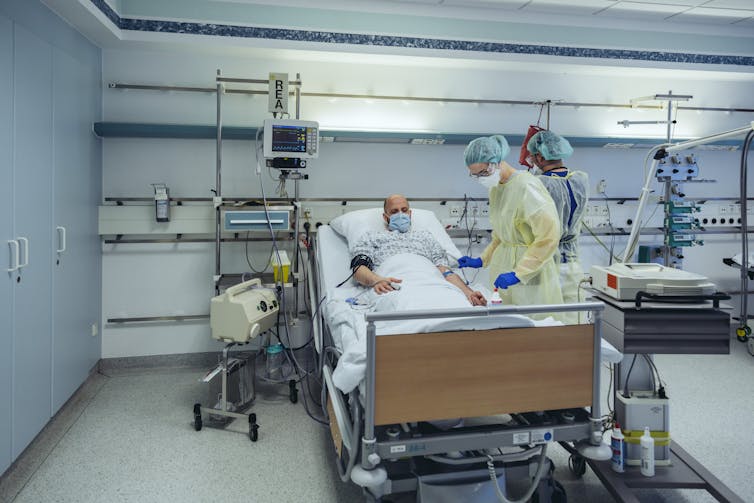
A few months ago, a young athletic guy came into my clinic where I’m an infectious disease physician and COVID-19 immunology researcher. He felt tired all the time, and, importantly to him, was having difficulty mountain biking. Three months earlier, he had tested positive for COVID-19. He is the kind of person you might expect to have a few days of mild symptoms before recovering fully. But when he walked into my clinic, he was still experiencing symptoms of COVID-19 and he could not mountain bike at the level he was able to before.
Tens of millions of Americans have been infected with and survived COVID-19. Thankfully, many survivors get back to normal health within two weeks of getting sick, but for some COVID-19 survivors – including my patient – symptoms can persist for months. These survivors are sometimes dubbed long-haulers, and the disease process is termed “long COVID” or post-acute COVID-19 syndrome. A long-hauler is anyone who has continued symptoms after an initial bout of COVID-19.
Numerous studies over the past few months have shown that about 1 in 3 people with COVID-19 will have symptoms that last longer than the typical two weeks. These symptoms affect not only people who were very sick and hospitalized with COVID-19, but also those with milder cases.
Long COVID is similar to COVID-19
Many long-haulers experience the same symptoms they had during their initial fight with COVID-19, such as fatigue, cognitive impairment (or brain fog), difficulty breathing, headaches, difficulty exercising, depression, sleep difficulty and loss of the sense of taste or smell. In my experience, patients’ symptoms seem to be less severe than when they were initially sick.
Some long-haulers develop new symptoms as well. These can vary widely person to person, and there are reports of everything from hair loss to rapid heart rates to anxiety.
Despite persistent symptoms, SARS-CoV-2 – the virus itself – is not detectable in most long-haulers. And without an active infection, they can’t spread the virus to others.
Who are the long-haulers?
Patients who were hospitalized for COVID-19 are the most likely to have persistent long-term symptoms.
In a study published in July 2020, Italian researchers followed 147 patients who had been hospitalized for COVID-19 and found that 87% still had symptoms 60 days after they were discharged from the hospital. A more recent study, published in January, found that 76% of hospitalized COVID-19 patients in Wuhan, China, were still experiencing symptoms six months after first getting sick.
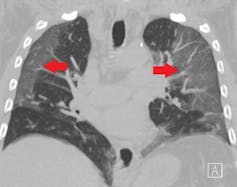
This Wuhan study was particularly interesting because the researchers used objective measures to evaluate the people reporting lingering symptoms. People in the study were still reporting persistent breathing problems six months after getting sick. When researchers performed CT scans to look at the patients’ lungs, many of the scans showed splotches called ground-glass opacities. These likely represent inflammation where SARS-CoV-2 had caused viral pneumonia. Additionally, the people in this study who had severe COVID-19 could not walk as fast as those whose illnesses were less severe – these lung problems reduced how much oxygen was moving from their lungs into their bloodstream. And remember, this was all measured six months after infection.
Other researchers have found similar objective health effects. One study found evidence of ongoing viral pneumonia three months after patients left the hospital. Another study of 100 German COVID-19 patients found that 60% had heart inflammation two to three months after initial infection. These German patients were relatively young and healthy – the average age was 49, and many had not needed hospitalization when they had COVID-19.
The sickest COVID-19 patients are not the only ones to suffer from long COVID. Patients who had a milder initial case that didn’t result in hospitalization can also have persistent symptoms.
[Deep knowledge, daily. Sign up for The Conversation’s newsletter.]
According to a recent survey done by the Centers for Disease Control and Prevention, 35% of nonhospitalized patients who had mild COVID-19 cases did not return to baseline health 14 to 21 days after their symptoms started. And this wasn’t just in older people or people with underlying health conditions. Twenty percent of previously healthy 18-to-34-year-olds had ongoing symptoms. Overall, research shows as many as one-third of individuals who had COVID-19 and weren’t hospitalized will still be experiencing symptoms up to three months later.
To put these numbers in context, only 10% of people who get the flu are still sick after 14 days.
Long-term symptoms, long-term effects
The medical community still does not know just how long these symptoms will persist or why they occur.
According to recent research that has yet to be peer-reviewed, many long-haulers cannot return to work or do normal activities because of brain fog, pain or debilitating fatigue. Before my patient got sick, he would bike up a mountain in our Colorado town almost every day. It took him four months to recover to the point where he could climb it again.
SARS-CoV-2 hurts people in more ways than the medical community originally recognized. At Colorado State University, my colleagues and I are studying long-haulers and exploring whether immune system imbalances play a part in their disease process. Our team and many others are diligently working to identify long-haulers, to better understand why symptoms persist and, importantly, to figure out how the medical community can help.![]()
Stephanie LaVergne, Research Scientist, Colorado State University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share of people living in poverty areas fell by 6.6 percentage points since first half of the decade
The share of the U.S. population living in poverty areas declined in the second half of this decade, dropping below levels a decade earlier, according to recent data.
The U.S. Census Bureau’s 2015-2019 5-year American Community Survey (ACS) shows the percentage of people in the United States living in poverty areas – defined as census tracts where at least 20% of the population lives in poverty – increased between 2005-2009 and 2010-2014. It then decreased in 2015-2019 to a lower level than in 2005-2009.
These changes reflect the broader economic trends of the last decade.
The data cover a 15-year period that included both the Great Recession (December 2007 to June 2009) and the subsequent period of economic expansion. Data collection for the 2015-2019 ACS concluded in December 2019, before the COVID-19 pandemic.
Living in communities with high poverty concentrations exposes residents to several challenges, such as poor housing conditions, limited job opportunities and high crime rates. Government programs often target resources to these high-poverty neighborhoods.
Poverty areas by state and region
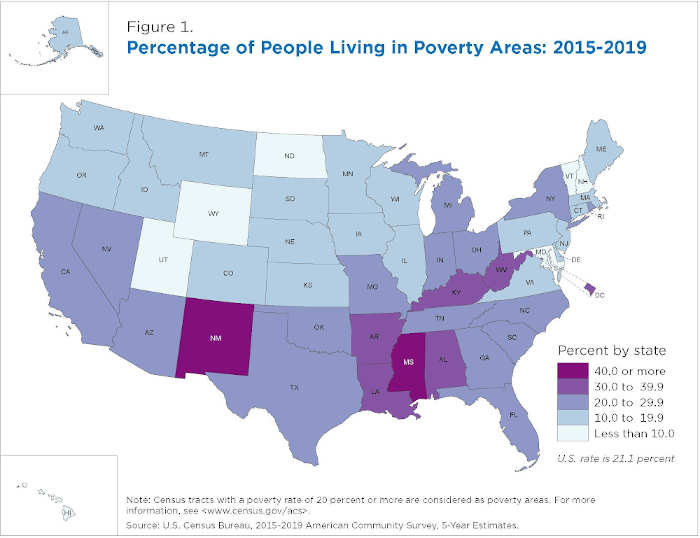
Figure 1 shows the percentage of people living in poverty areas varied in the states with some sharp regional differences.
The Census Bureau defines four regions: Northeast, South, Midwest and West. Six of the seven states with over 30% of their population living in poverty areas were in the South region.
In the 2015-2019 period:
– 21.1% of the U.S. population lived in poverty areas, ranging from a low of 5.2% in New Hampshire to a high of 42.4% in Mississippi.
– In seven states, all in the South except for New Mexico, and the District of Columbia, at least 30% of residents lived in high poverty areas. In Mississippi and New Mexico, at least 40% of people lived in high-poverty areas.
– In seven states, 10% or less of the population lived in poverty areas. These states were spread across the country: three in the West, two in the Northeast, one in the South and one in the Midwest.
The percentage of the U.S. population living in poverty areas changed during the 15-year period stretching from 2005 to 2019.
In the 2005-2009 period, 21.3% of the nation’s population lived in poverty areas. During the 2010-2014 period, this increased by 6.4 percentage points to 27.7%. The rate then declined by 6.6 percentage points to 21.1% in the 2015-2019 period.
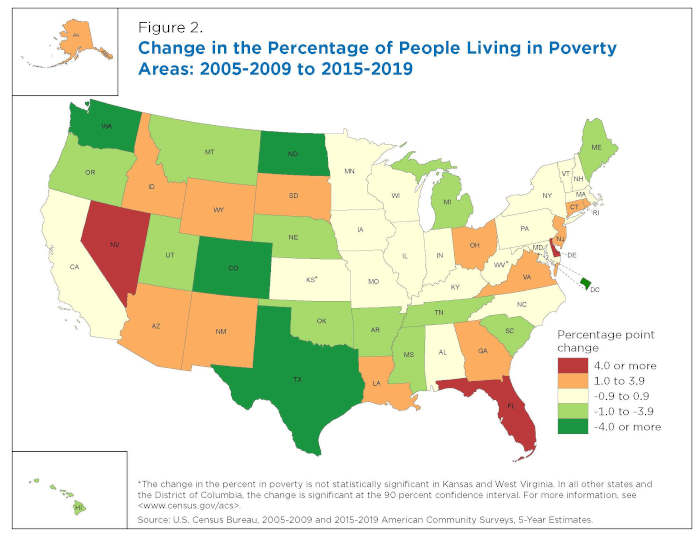
From 2005-2009 to 2015-2019, the percentage of people living in poverty areas in the United States fell by 0.2 percentage points. But there was more variation between these two time periods at the state level (Figure 2).
From 2005-2009 to 2015-2019:
– The percentage of people living in poverty areas increased in 25 states and decreased in 23 states and the District of Columbia. The change was not statistically significant in two states.
In three states — Nevada, Delaware and Florida —the percentage of the population living in poverty areas rose by more than four percentage points.
– In four states (Washington, North Dakota, Colorado and Texas), the slice of the population living in poverty areas dropped by four percentage points or more.
The report, Changes in Poverty Rates and Poverty Areas Over Time: 2005 to 2019, provides more information on changes in poverty areas in the United States. Percentage of People in Poverty by County: 2015-2019 is an interactive visualization that shows changes in county level poverty rates by Hispanic origin and race.
Em Shrider and Craig Benson are survey statisticians in the Poverty Statistics Branch.
The following dogs are ready for adoption or foster.

‘Agatha’
“Agatha” is a female Rhodesian Ridgeback mix with a short red and black coat.
She is dog No. 4603.

‘Boog’
“Boog” is a male Rottweiler with a short black coat.
He is dog No. 4609.

‘Breeze’
“Breeze” is a female American Pit Bull Terrier mix.
She has been spayed.
She is dog No. 4445.
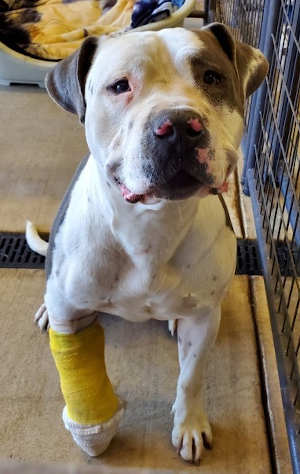
‘Dorito’
“Dorito” is a male American Staffordshire Terrier mix with a short white and gray coat.
He has been neutered.
He is dog No. 4576.

‘Inky’
“Inky” is a male German Shepherd mix with a long black coat.
He has been neutered.
He is dog No. 4324.

Jerry
“Jerry” is a male pit bull terrier mix with a short brindle coat.
He is dog No. 4455.

‘Mommas’
“Mommas” is a female American Pit Bull terrier mix with a white coat.
She has been spayed.
She is dog No. 4499.

‘Rudolph’
“Rudolph” is a male shepherd mix.
He has a short tan and black coat.
He is dog No. 4436.

‘Scooter’
“Scooter” is a male shepherd mix puppy.
He has a medium-length tan and white coat.
He is dog No. 4649.

‘Tiabeanie’
“Tiabeanie” is a female American Bully with a short black with white markings.
She is dog No. 4602.

‘Toby’
“Toby” is a friendly senior male boxer mix.
He has a short tan and white coat.
He is dog No. 4389.
Call the Clearlake Animal Control shelter at 707-273-9440, or email
Visit Clearlake Animal Control on Facebook or on the city’s website.
Email Elizabeth Larson at
The National Weather Service’s Eureka office said another round of rain will arrive Thursday and continue across the region through Saturday morning, when colder air is forecast to arrive.
Snow levels could rise from 2,500 feet to over 6,000 feet, especially near the coast, the forecast said.
Across the North Coast, rainfall amounts will range from a half-inch to an inch in most areas with higher amounts in the mountains. Less than a quarter inch is expected in much of Lake County, forecasters said.
The Lake County forecast calls for less than a tenth of an inch of rain Thursday night, with rain again on Friday and into Friday night.
On Friday, winds with gusts topping 21 miles per hour are expected across Lake County, the forecast said.
During the day on Saturday, conditions are expected to be mostly sunny, with single-digit winds, and patchy fog on Saturday night into Sunday morning.
Sunday and Monday will be clear, then the forecast calls for times of patchy fog from Monday night through Wednesday, then clearing to mostly sunny conditions.
Daytime temperatures through Saturday are to be in the low 50s, rising into the 60s next week. Nighttime conditions will hover in the high 30s and low 40s.
Email Elizabeth Larson at
 How to resolve AdBlock issue?
How to resolve AdBlock issue? 