News
- Details
- Written by: Stella U. Ogunwole, Megan A. Rabe, Andrew W. Roberts, And Zoe Caplan
In 2020, the U.S. Census Bureau counted 331.4 million people living in the United States; more than three-quarters (77.9%) or 258.3 million were adults, 18 years or older — a 10.1% increase from 234.6 million in 2010.
The aging of baby boomers, those born between 1946 and 1964, who were ages 57 to 75 in 2021, is partly driving the growth in the adult population.
The 2020 Census shows that the Northeast had the largest proportion of adult population (79.7%) and the smallest proportion of people under age 18 (20.3%).
In contrast, the South had the lowest proportion of adult population (77.5%) and the highest proportion of young population (22.5%).
By comparison, the younger population under age 18 numbered 73.1 million, or 22.1% of the U.S. population in 2020, a 1.4% decrease from 74.2 million in 2010. The slow decline of the younger population is in part due to a general decrease in fertility, ongoing since 2007.
During the same period, the total U.S. population grew at a slower rate than the adult population: up 7.4% from 308.7 million in 2010 (Table 1).
Although the adult population grew from 2010 to 2020, the growth was lower than in the first decade of the 21st century when it grew 12.2%, to 234.6 million in 2010 from 209.1 million in 2000.
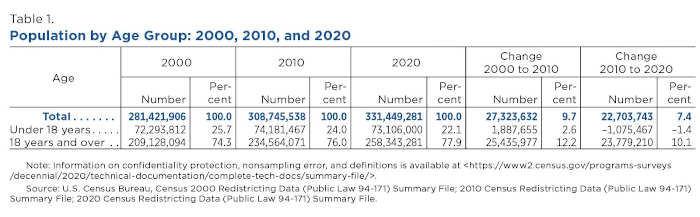
Adult population in the West shows fastest growth, south had largest increase
The 2020 Census shows that the Northeast had the largest proportion of adult population (79.7%) and the smallest proportion of people under age 18 (20.3%) (Table 2a).
In contrast, the South had the lowest proportion of adult population (77.5%) and the highest proportion of young population (22.5%).
But only the South maintained growth in both age groups from 2000 to 2010 and 2010 to 2020: The young population in that region increased by 2.2 million (8.7%) and by 0.6 million (2.1%), respectively (Table 2b).
The adult population in the South also experienced the largest numeric increase of 11.1 million, or 12.8%, between 2010 and 2020.
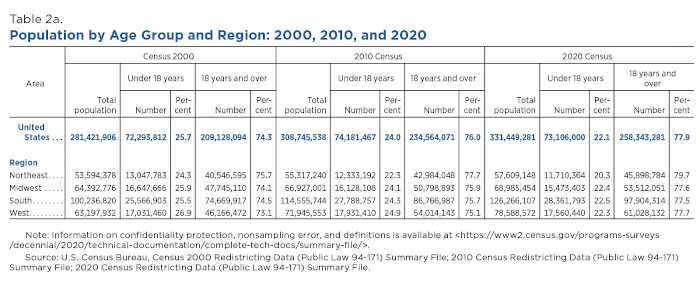
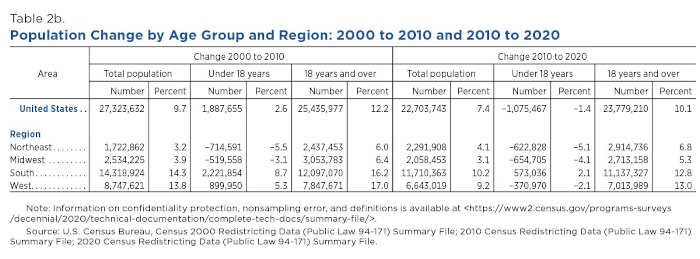
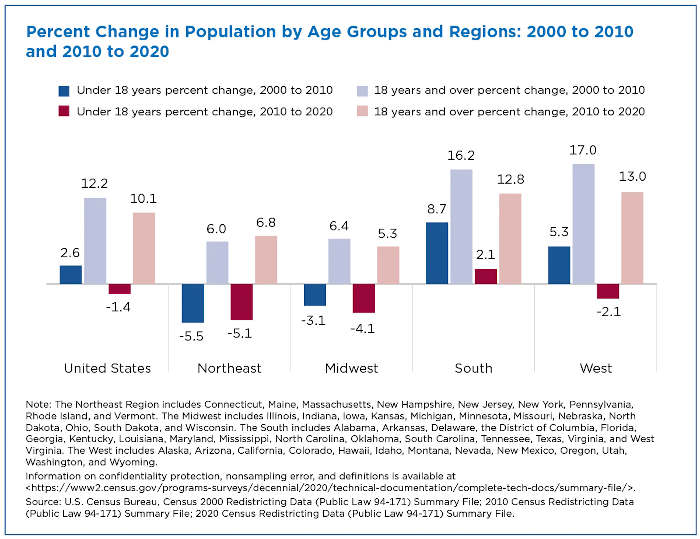
The figure below shows that the adult population grew in all regions during the 2000s and 2010s. The West experienced the fastest population change between 2010 and 2020, adding 7 million (13%) adults.
However, the Northeast was the only region where the adult population grew faster between 2010 and 2020 (6.8% or 2.9 million) than between 2000 and 2010 (6% or 2.4 million).
In the rest of the regions and across the country, the adult population grew at a slower pace over the last decade. The younger population also grew more slowly or declined.
Use this interactive data visualization to learn about the size, growth rate and distribution of the adult and under-age-18 populations in your state and county.
Stella Ogunwole, Megan Rabe and Zoe Caplan are demographic statisticians in the Sex and Age Statistics Branch in the Census Bureau’s Population Division. Andrew Roberts is chief of the Sex and Age Statistics Branch.
- Details
- Written by: Lilly Cheng Immergluck, Morehouse School of Medicine

With the delta variant making up over 93% of COVID-19 cases in the U.S. at the end of July 2021, questions arise about how to stay protected against evolving forms of the SARS-CoV-2 virus. Here, pediatrician and infectious disease specialist Dr. Lilly Cheng Immergluck of Morehouse School of Medicine answers some common questions about variants and what you can do to best protect yourself.
1. What are variants and how do they emerge?
Viruses mutate over time to adapt to their environment and improve their survival. Over the course of the pandemic, SARS-CoV-2, the novel coronavirus that causes COVID-19, has mutated enough to change both its ability to spread through the population and its ability to infect people.
These new strains are called variants. The U.S. Centers for Disease Control and Prevention currently classifies variants into three categories, listed in order of least to most concerning:
-
Variant of Interest (VOI): Have features that may reduce your immune system’s ability to prevent infection. For example, you might have heard of VOI eta, iota or kappa.
-
Variant of Concern (VOC): Are less responsive to treatments or vaccines and more likely to evade diagnostic detection. They tend to be more transmissible, or contagious, and result in more severe infections. Alpha and delta are VOCs, for instance.
-
Variant of High Consequence (VOHC): Are significantly less responsive to existing diagnostic, prevention and treatment options. They also result in more severe infections and hospitalizations. There have not been any VOHCs identified so far.
The World Health Organization uses similar classifications, but their definitions may differ from the CDC’s U.S.-based ones, as variant features and effects may differ by geographic location.
2. Are variants always more harmful?
A variant may be more or less dangerous than other strains depending on the mutations in its genetic code. Mutations can affect attributes like how contagious a viral variant is, how it interacts with the immune system or the severity of the symptoms it triggers.
For example, the alpha variant is more transmissible than the original form of SARS-CoV-2. Studies show it’s somewhere between 43% to 90% more contagious than the virus that was most common at the start of the pandemic. Alpha also is more likely to cause severe disease, as indicated by increased rates of hospitalization and death after infection.
Even more extreme, the delta variant is reported to be nearly twice as contagious as previous strains and may cause even more severe disease among those who are unvaccinated. The viral load of those infected with delta – meaning the amount of virus detected from the nasal passages of an infected person – is also reported to be over 1,000 times higher than in those infected with the original form of SARS-CoV-2. Recent evidence also suggests that both unvaccinated and vaccinated people carry similar viral loads, further contributing to the especially contagious nature of this variant.
3. Which variants are most common in the US?
Over the course of a few months, the delta variant has become the predominant strain in the U.S., accounting for the vast majority of COVID-19 cases at the end of July 2021.
But there are regional variations across the country. As of July 31, the CDC estimated that the alpha variant represented over 3% of cases identified in a region of eight states that includes Georgia, Florida and Tennessee, compared with less than 1% in the region that includes Iowa, Kansas, Missouri and Nebraska. The CDC tracks variants in cooperation with state health departments and other public health agencies. COVID-19 infection samples from across the country are genetically sequenced each week to identify existing and new variants.
And new variants will likely continue to appear as the virus evolves. Delta plus, for instance, is a sub-lineage of delta. The effects of this subvariant are yet to be determined.
4. How are vaccines holding up against variants?
Researchers are working to figure out how effective the three COVID-19 vaccines currently authorized for emergency use in the U.S. are at preventing infection from variants in “real-world” conditions where variant distribution and frequency constantly change. Several preliminary studies that have not yet been peer-reviewed suggest that these vaccines are still effective in preventing COVID-19-related serious infections and death.
No vaccine is perfect, however, and breakthrough COVID-19 infections are possible in those who are vaccinated. Older adults and those with immunocompromising conditions may be at increased risk to have these breakthrough infections.

Thankfully, fully vaccinated individuals generally experience milder COVID-19 infections. For example, a study analyzing COVID-19 cases in England estimated that two doses of the Pfizer BioNTech vaccine are 93.7% effective in preventing symptomatic disease from the alpha variant and 88% effective from delta. A different study in Ontario, Canada, that is not yet peer-reviewed reported that the Moderna vaccine is 92% effective in preventing symptomatic disease from alpha.
5. How can I stay safe?
How cautious you should be depends on a number of individual and external factors.
One factor is whether you’re fully vaccinated. Nearly all - 99.5% - of COVID-19 deaths in the U.S. over the past few months were among unvaccinated people.
The most recent CDC guidelines recommend that everyone wear a mask in areas of substantial or high transmission, regardless of whether or not they’re vaccinated. More caution should especially be taken if you aren’t fully vaccinated or have a weakened immune system.
[Understand new developments in science, health and technology, each week. Subscribe to The Conversation’s science newsletter.]
Another factor to consider is the level of community transmission and the proportion of unvaccinated people in your local community. For example, someone who lives in an area that is below the national average for COVID-19 vaccinations may have a higher chance of encountering someone who is unvaccinated – and so more likely to spread the coronavirus – than someone in an area with higher vaccination rates.
Finally, there are still a significant number of people who are at high risk of COVID-19, including children. As of Aug. 3, 2021, only 29.1% of children ages 12 to 15, and 40.4% of those ages 16 and 17, had been fully vaccinated. The American Academy of Pediatrics and the Children’s Hospital Association note that 4,292,120 total child COVID-19 cases had been reported as of Aug. 5. Children make up 14.3% of reported COVID-19 cases. If your child is unvaccinated, the best way you can protect them and other unvaccinated members of your household is to get yourself vaccinated and have everyone wear a mask in indoor public spaces.
Guidelines provided by public health agencies are simply that – general guidelines. They are not tailored to be prescriptive for each individual and their personal risk assessments.
Vaccines remain the best protection against every strain of the novel coronavirus. But masking, social distancing and avoiding crowds and poorly ventilated indoor spaces add extra layers of protection against breakthrough infections and lower your risk of inadvertently spreading the virus.![]()
Lilly Cheng Immergluck, Professor of Microbiology, Biochemistry and Immunology, Morehouse School of Medicine
This article is republished from The Conversation under a Creative Commons license. Read the original article.
- Details
- Written by: Elizabeth Larson

LAKE COUNTY, Calif. — A blown tire led to a cement truck crash and rollover on Thursday morning near Kelseyville, but the driver escaped serious injury.
Gerardo Martinez, 59, of Kelseyville, suffered minor injuries in the crash, the California Highway Patrol’s Clear Lake Area office reported.
At 9:35 a.m. Thursday, Martinez was driving a 2001 Peterbilt cement truck southbound on Highway just south of Bottle Rock Road at 40 to 45 miles per hour, the CHP said.
The CHP said Martinez told officers that the truck's right front tire blew out, causing him to lose control.
Martinez drove off the west roadway edge of Highway 29 and hit the west dirt embankment. The CHP said the truck ended up on its left side, partially blocking the southbound lane.
The CHP said the truck was fully loaded with cement at the time of the wreck, however, no cement spill was reported.
Kelseyville Fire transported Martinez to Sutter Lakeside Hospital for treatment of minor injuries, the CHP said.
The report said Martinez was using his safety equipment at the time the wreck occurred.
This CHP said the crash remains under investigation.
Email Elizabeth Larson at
- Details
- Written by: Elizabeth Larson
The California Department of Public Health on Wednesday issued a public health order requiring all school staff to either show proof of full vaccination or be tested at least once per week.
The state said the new policy takes effect Thursday, Aug. 12, and schools must be in full compliance by Oct. 15.
“It is a surprise,” Lake County Superintendent of Schools Brock Falkenberg said of the new vaccination and testing mandate.
“We as educators are planners, and we like to just follow the plan,” he said.
In this case, there was little time to plan or prepare for the new rules the state handed down this week.
Falkenberg told Lake County News that, normally, when such orders or mandates are about to be released, he’ll get several days’ worth of warnings.
However, in this instance, he got the first notice about the impending public health order announcement at 11 p.m. Tuesday.
“We are still trying to look at the details of what was said and what is the California Department of Public Health order, because that’s really what counts,” Falkenberg said Wednesday evening.
“We’re still trying to really understand that language,” and understand how it will impact the Lake County Office of Education and all of the county’s districts and schools, he said.
Once they get a better understanding of the mandate, Falkenberg said the Office of Education will provide guidance and support to the county’s school districts.
The state’s new health order comes as Lake County schools are welcoming students back to class for the new academic year.
Lakeport Unified, Lucerne Elementary and Upper Lake Unified had their first day of school on Wednesday, with Konocti Unified and Middletown Unified set to return on Aug. 16 and Kelseyville Unified on Sept. 7.
Falkenberg said he visited every campus on Wednesday where classes had started and there was great school turnout.
In Lucerne and Upper Lake, schools had been open all of last year. “Their families have already been through this,” said Falkenberg, noting the schools have invested the time and energy to develop that trust. “Their turnout is very, very high for face-to-face instruction.”
Falkenberg said he’s interested to see what turnout is like in other districts that were only in session for a matter of months last year. “We don’t know what those numbers look like yet.”
While Lakeport schools looked very well attended on Wednesday, he said it was the first day of school, and enrollment numbers are not required to be submitted by districts until the first week of October. At that time, a clearer picture should emerge of school enrollments.
Making adjustments
“Every county, every community is different,” said Falkenberg, and small counties like Lake have decisions imposed on them by the state that are really meant to impact larger counties.
As the Office of Education works on understanding the new mandate, one of the questions already coming up is who will pay for it.
That was a question raised by the Lake County Board of Education, which had a regular meeting on Wednesday.
During his report to the board, Falkenberg updated trustees on the new guidance and they asked him about who will pay for testing.
He said the state will, in fact, cover those costs.
Falkenberg said Lake County’s schools and Public Health have built a strong working relationship around pandemic-related issues, discussing requirements and needs, and creating partnerships to meet them.
The districts have worked with Public Health to provide rapid tests and Public Health has supported the schools with free testing. Now, however, Falkenberg said to continue to get free testing, schools need to go through the California Department of Education. The only cost to schools is for the shipping.
The new vaccination guidance, however, doesn’t take into account the limited number of school nurses, said Falkenberg.
“School nurses are in short supply across the state,” and even the Office of Education doesn’t have its own nurse, he said.
“The cost of time, coordination and resources to do the testing is certainly something the districts will have to bear,” although Falkenberg said the state and federal governments have provided an ample amount of funding to work testing into school plans.
The vaccination effort
The effort to get vaccinations for those teachers and school staff who wanted them has been going on for many months.
“The county Office of Education coordinated with public health to fill all available slots in January and February with educators, school staff, including the community college staff, and eventually our preschool and child care staff,” said Falkenberg.
At one point, he said they had an idea of the number of staff members from each district that wanted to be vaccinated, but did not have a list of names. “We didn’t want a name as an agency, we just wanted numbers.”
Falkenberg said the Office of Education worked with district superintendents to develop an equitable plan of vaccine distribution around the county.
They wanted to meet the needs of those in front of students first, so they started with Lucerne and Upper Lake school staffs, as they were back to in-person classes before the other districts.
On Wednesday, Falkenberg said he didn’t know how many individuals actually followed through and got vaccinated or who got vaccinated since then and didn’t’ come through the schools’ sign-up process. “I don’t know that anyone has that number.”
In addition, following guidance from the California Department of Public Health and Cal/OSHA, Falkenberg said the Office of Education entered into a process to allow office staff to start removing masks by either showing proof of vaccination or other medical reasons for not masking.
Based on the new guidance, Falkenberg said the districts need to know who has been vaccinated. “That's the first step that needs to happen.”
He said county superintendents have regular Friday lunch Zoom meetings and he expects the new vaccination guidance will be a key topic of upcoming meetings.
In a letter to parents issued on July 30, interim Lake County Public Health Officer Dr. Charlie Evans said vaccination rates for children ages 12 to 19 was 19%. “When schools resume, all
students will be asked to mask while indoors, until we reach an immunity level through vaccination that is enough to sustain us at a very low infection rate.”
Evans asked parents to take their children who qualify for vaccination to their primary care doctor or a vaccination clinic for evaluation and treatment with the COVID-19 vaccine, which he said was the primary method of helping Lake County achieve the goal of keeping schools open for in-classroom teaching throughout the year.
He also asked people to follow the “Three Ws” — “Wear a mask. Wash your hands. Watch your distance.”
The Office of Education put together vaccination and testing teams several months ago. Falkenberg said the vaccination team focuses on 12- to 18-year-olds but will vaccinate anyone who shows up who wants the shot, he said.
Falkenberg said the testing team was formed as a partnership between the Office of Education, Lucerne Elementary, Upper Lake Unified and the Lake County International Charter School, and he said they’ve been providing testing as requested for many months.
One of Falkenberg’s immediate concerns is how the new mandate will impact those vaccination and testing teams.
Now that either vaccination or testing is required, Falkenberg said the question is whether they will be able to support that team, which is why they need to find out how many people have been vaccinated.
“I think a lot is going to become more evident over the next day or two,” Falkenberg said.
Email Elizabeth Larson at
 How to resolve AdBlock issue?
How to resolve AdBlock issue? 